To Port Or Not To Port

When I think of the word “port,” my mind naturally goes to a place where a cruise ship pulls in for passengers to get off the boat, or perhaps where our country receives imports from other countries. But for today’s cancer patients, a “port” is a device that makes administering chemotherapy so much easier, and comfortable.
For survivors like me, we did not have the option of a port to administer chemo. But as you read my book “Paul’s Heart – Life As A Dad And A 35-Year Cancer Survivor” (available on Amazon), the port is another great progress made in treating cancer.

The question came from one of my feeds for current Hodgkin’s Lymphoma patients. ”Are you able to opt out of having a port for treatment?” This seems like a perfect question to ask by someone with no experience in cancer, and also likely to not have had any kind of surgery previously. The port is placed under the skin, which requires surgery. So, that of course is scary. And because diagnosis and staging is done with less surgeries than when I was treated, unlike just being another surgery for me, this can be overwhelming.
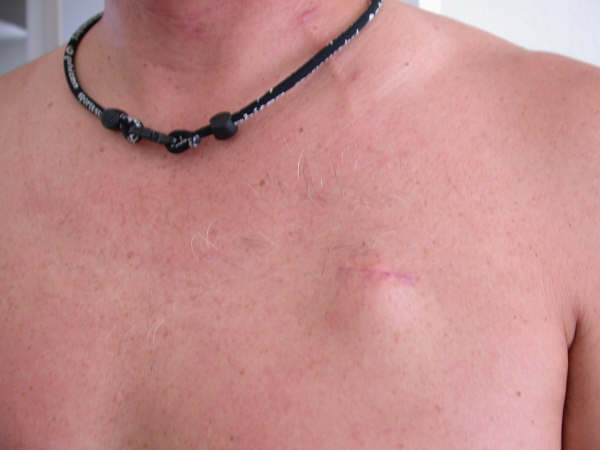
Typically, once placed, the only ones who will be aware that you have a port, is you, your oncologist, and your oncology nurse administering the chemo. Except for a bump or some raised skin, underneath your clothing, it is not visible to anyone else. So cosmetically it does not harm.
Here is the true benefit. Chemotherapy wreaks havoc on the veins, irreparable damage. I am not going to get all nerdy and scientific, as my experience and history explain it pretty well enough. I simply have no surface veins left for even a simple blood draw for a normal non-cancer blood test. As I went through each treatment, more and more veins became less usable. This also meant more “needle sticks” to find other veins.
Of course, I did get through my treatments, without ports being available yet. But now, here is how a simple blood draw goes for me. I walk into a lab. I sit in the chair. And the phlebotomist or tech asks me my name. I say, “Paul Edelman. I am a 33 year survivor of Hodgkin’s Lymphoma with chemo-ravaged veins. I am a hard stick. So I am going to ask you to use a “butterfly gauge” needle, and if you are able to find a vein, only if you are confident that you can hit it, then go for it. Otherwise don’t. I develop major anxiety with multiple sticks. If you don’t think you can do it, ask someone who might have more experience, or if you can use doplar to locate a deeper vein. I don’t mind. I actually prefer that.”
Even if you were not the one drawing blood from me, would you want that kind of pressure put on you? Would you be irritated with the whininess? Would you do all you can to prevent a panic attack that will begin with draw attempt number three? This has been my life for thirty-five years now. My daughters have always been better with blood tests than me. I do not bother with being embarrassed. I combine all my blood tests to be done at the same time. And there is only one place that I have confidence in the staff to listen to me. I have actually been in the ER with nurses who refused to even try because they knew what I was talking about.
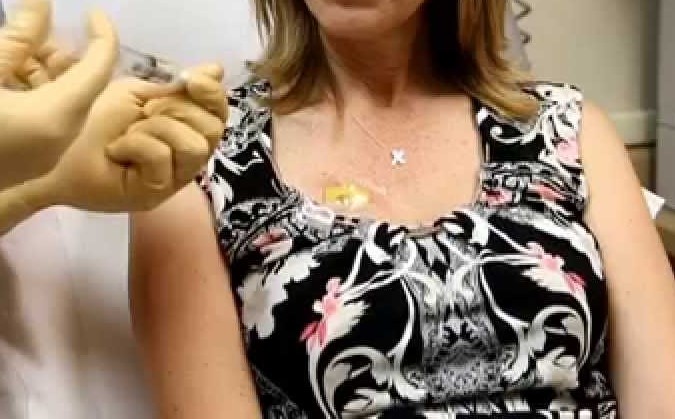
I would not be in this situation today, if I had the option to have a port, and have my chemotherapy administered that way. There would be no seek-and-destroy veins, just the constant dose into the same location. No stress, no anxiety.
I really cannot on the port itself since I did not have one. My father had one placed when he was treated for his lung cancer. But the overwhelming response to the writer was in support of getting a port. You could see an understand the writer was apprehensive, possibly scared. We do not come into cancer with experience, normally unless a patient has relapsed or developed another cancer. And “back in the day,” there was no social media to seek peer advice on what to do.
While there were a minority of patients who toughed it out without a port, the majority of patients expressed relief with having had the port placed. One response actually mentioned one of the only times a port might not be considered, and that is if the surgery and recovery were to delay treatment beyond any reasonable timing.
The important thing to keep in mind, just as the situation with cancer itself, the port is not permanent. The port will eventually be removed after a certain amount of time that chemotherapy is completed. The difference between those with ports and me? Those with ports will still have working veins for routine bloodwork.







