When The Body Tries To Warn You – Part 3
I arrived by 5:30am as instructed for my 6:30am procedure, to have at least one blockage, possibly more, to be stented via trans catheterization, simpler put, fixing my heart through my leg. As opposed to doing this by open heart surgery which would take weeks if not months to recover, this is why Dr. S said he would have me up and going in a week or two.
My nurse’s name was Heather. She took me back to a holding area, for me to get changed into a hospital gown. And then, again probably the most stressful part of my procedures, trying to get an IV into my arm, you want your best tech to have at me, not one who draws the shortest straw. I had gotten real good at warning techs and nurses that I am a hard stick due to my chemo history, that back when I was treated for Hodgkin’s Lymphoma, ports were not an option (so there, here is my PSA… GET A PORT IF THEY OFFER IT TO YOU!!! It is not worth being stabbed repeatedly trying to find a working surface vein.).
Everything was going smoothly, and quickly. Heather would pop back in frequently to see if I was comfortable or if I needed anything (as in to calm down). I cannot say what prompted me, but I brought up a totally unrelated conversation. “This is the first time I am having anything done since I was diagnosed with Hodgkin’s Lymphoma back in 1988.” I had Heather’s interest. “I went through radiation therapy and chemotherapy, and have been in remission ever since.” Heather’s face showed more than a little intrigue, she had something in her thoughts, and it was serious. I assured her that I was fine, the only lasting issues that I had from it, was that I was not able to biologically have kids, my thyroid was messed up, and that I had no spleen from my laparotomy, so doctors need to take extra precautions to make sure I don’t contract any infections. She wrote down that I was “asplenic”, without a spleen. Turns out this was an important detail (as with any surgery for me). Heather said, “that’s good to know because it is important. We will probably get some prophylactic antibiotics into you before starting.” Okay, made no difference to me. They were the professionals and I had all my trust in them.
At that point, I was given a sedative as I remember nothing after that.
When the procedure was finished and I came to, groggily, I was in a private room. There was Dr. S and a friend of mine who had stopped by to check up on me. My head was woozy, so I know it was hard to focus on what Dr. S was trying to explain. Even with newer pictures and a drawing, I could barely make sense of it, not to mention, apparently take it seriously.

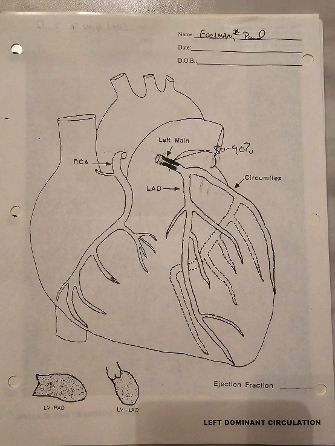
“We were unable to do the stents as the cath revealed extensive scarring to the left anterior descending artery, producing a 90% blockage.” Just then, my friend, who happened to be a paramedic and also happened to recognize in plain English what the doctor just explained medically, blurted out, “oh my God, a ‘widow maker’!” Dr. S interrupted, “yes, but we don’t like to refer to it as that. Paul actually has two other blockages to be dealt with as well, so I have him set up for an emergency triple bypass first thing in the morning.”
I kind of heard everything, but understood nothing. Out of the word “bypass,” I got the word “by” out if it, and just started babbling, “bypass? bye-bye. bye-bye bypass…” At this point, I do remember the clock on the wall saying 3:00. Dr. S left the room, and I nodded back off to sleep.
I woke up a little just after 4pm, not nearly as groggy as I was. On the table next to my hospital bed, were the two sheets pictured above, the photo and the diagram. I remembered vaguely what these things represented. Just then a nurse came in. Clearly I was confused as to what was going on. I had pain in my leg where they went in to do the catheterization (and failed). The nurse recommended that I stay in bed until the cobwebs were definitely gone from my head, and the pressure had gone down in the incision in my leg. I asked the nurse what happened and what was going on.
She explained that when they went in through my leg up to my heart, they discovered that my cardiac system had been so badly scarred from the radiation therapy I underwent back in 1989, making it impossible to implant stents to open up the blockages. There was the worst blockage, the one that was 90%, the LAD or “widow maker,” another that was 40% blocked, and the third, with the right coronary artery (RCA) blocked 30%. I was set for an emergency triple bypass at 6:30am. My head may have been clearer from the anesthesia, but still I was not reacting to this news the way I should have been. I was focused on one thing, two actually, my daughters.
My daughters were only three years old and five years old at this time, but already they had been exposed to the situation of having friends who had lost a parent. Of course, even at their young age, and explained age-appropriately, they still understood the loss their friends experienced, never to see their dad again. And I began to cry. I did not want to die. The nurse tried to console me, eventually giving me something to calm down as I was getting worked up over the situation. There was a lot that was going to happen over the next several hours, pre-op to be done, as well as get my one and only meal in, as I would be fasting as of 8pm for my early morning surgery. The last thing I felt like doing was eating. All I could think about was my daughters.
Just like that it started, in came phlebotomists to draw blood, a wheelchair to take me for an ultrasound of my legs to see which veins or arteries could be harvested for my bypasses. Everything was happening quickly now. And with my head clear, I was also paying attention now to everything being said around me. Up and down both legs they went with the ultrasound wand and a standard thick sharpie, outlining my veins on each leg that they felt were suitable for harvesting. Then it was off to x-ray for a chest pic and an echocardiogram.
I got back to my room around 6:00, food was waiting for me. I did not feel like eating, nor did I think it would make any difference as the next day was going to be without food anyway, well, at least orally. All I could think about was wanting to talk to my daughters. I had to reach them some time before they went to bed. I needed them to know what was going on, what to expect, on a small child level. I had to be careful how I explained everything so as not to scare them, not wanting to remind them of their friend’s father who passed away from a heart attack.
I got ahold of them just before 8:00 when they would be heading to bed. I told them, that I was seeing doctors who wanted to fix me up. They are very nice to me, and have a good plan that after the next day, I will be good as new, and that I would be home a few days after that. Not to worry about me. I was going to be fine. This was the second night in a row I had not seen them, been able to hug and kiss them goodnight. But I let them know how much I loved them and could not wait to see them again soon. The doctors would make sure of that.
I held myself together while I was on the phone with my daughters, and broke down immediately as soon as I hung up. Somehow, I was lacking the confidence that I clearly portrayed to my daughters. A nurse came in and asked if there was anything she could get me, and I said I just had one favor. If there was any chance that I could get a ride down to the hospital chapel. I am not an organized practitioner of religion, but I have my faith. And I wanted to make sure my surgeons were being watched over, and my daughters were being watched over. And of course, if there was anything that could be done to get me through the surgery.

(photo courtesy of IMDB)
At 3am, a huge man, who resembled Michael Clarke Duncan, dressed in green scrubs came into my room. He was there to prep me for my surgery. He would also be my valet to the chapel, and eventually downstairs to the operating room. Just like Duncan’s character in the Green Mile, he was a gentle giant of a man, towering over me. I was beginning to think my age and what I was about to undergo was having an impact on those taking care of me.
5:30am rolled around, and into the room came a gourney instead of a wheelchair this time. Some extra help came into the room, to lift me from my bed onto the gourney. It was go time.
